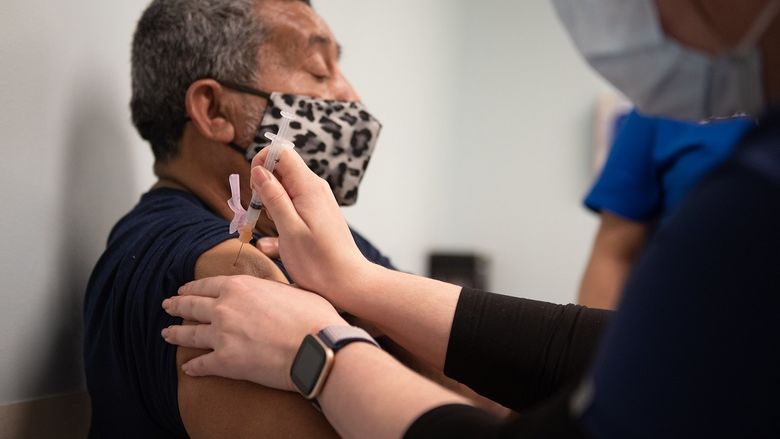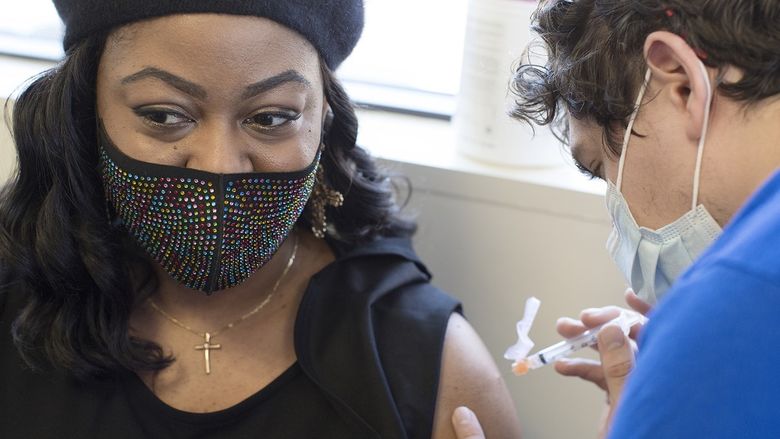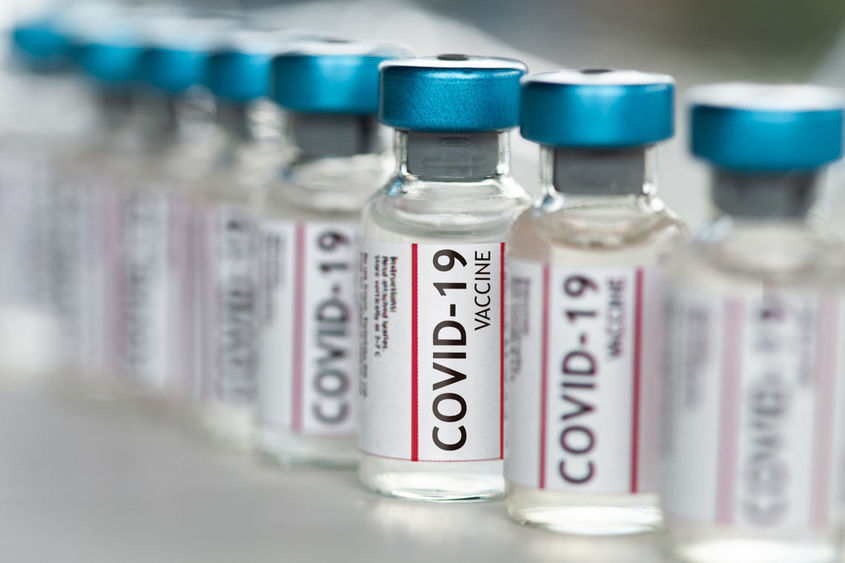
Manufacturers hope to distribute 200 million doses of COVID-19 vaccines in the coming months.
ERIE, Pa. — For shipping companies, the most complicated step in any delivery process is often the “last mile” — the transfer of packages from a distribution center to individual customers. In the months ahead, that process will be tested as never before in peacetime America, with the distribution of 200 million doses of the new COVID-19 vaccines.
We asked Varun Gupta, associate professor of supply chain management and analytics at Penn State Behrend, how distribution of the vaccines will be managed, how the scale of the initiative will complicate the effort, and how confident we can be that the process will work, considering the recent scarcity of even basic products, such as toilet paper.
The nation is undertaking a significant logistical challenge: Transporting, distributing and administering a vaccine to hundreds of millions of Americans who are desperate to receive it. What’s the model for making that work?
Gupta: The process we’re seeing now is different from traditional supply chains, where efficiencies are usually realized as cost savings. The main goal for distributing the COVID-19 vaccines should be to have a high throughput across the supply chain, so that a minimal amount of the product — the vaccine — is wasted.
For that reason, these operations are being set up like wartime and humanitarian logistics, where the U.S. Army and the Marines build highly responsive supply chains to meet the demand at any cost. It should not be a surprise, then, that the chief of Operation Warp Speed is a U.S. Army general, Gustave F. Perna.
This is a federal initiative, with a public component — the shipping companies, including UPS — and a reliance on the states to determine how and when people will be vaccinated. If that process breaks down, is there a stage at which you would anticipate that occurring?
Gupta: The allocation between states will be challenging.
More importantly, any delay or variation typically spreads along a supply chain. That may lead to vaccines being wasted, if more doses than are required are shipped to some locations.
There is a lot of emphasis now on transparency and the ability to track shipments and the administration of vaccines in real time. As the supplies increase and more groups are eligible to receive vaccines through different channels, such as pharmacies, doctor’s offices and county health departments, we will likely see shortages and difficulties in moving those shipments quickly enough.
The vaccines need to be transported and stored at sub-zero temperatures. How much does that complicate the distribution effort?
Gupta: Any breakage in the cold supply chain can render the vaccine ineffective. That will lead to waste.
So far, the Pfizer vaccine has been transported successfully, using dry ice to maintain the temperature in special boxes. It will be interesting to see if that can be scaled up, as there could be supply issues with dry ice, the special boxes and the trucks that can transport them safely.
Moderna’s vaccine can be stored and transported using traditional cold-storage supply chains, which are already well-developed and have higher handling capacities. At this point, I am more concerned about the ability of those administering the vaccine to be able to safely handle two different vaccines at different temperatures.
How will Pfizer and Moderna ramp-up production of their vaccines, which have now been approved for use? How quickly can they do that?
Gupta: That’s going to be a challenge. Companies often increase production by securing capacity at other vaccine manufacturers, or by buying smaller companies. In this case, however, the need to maintain quality standards for a novel vaccine may limit their ability to exponentially increase production.
Do you anticipate any problems producing or securing related materials, such as vials or packaging?
Gupta: Vials and shipping cartons should not bottleneck the production, as a majority of these are manufactured domestically. The specialized storage boxes and PPE items, such as gloves or safety masks, could present a bigger challenge in the long term, and in large quantities. There already is a latex glove shortage, due to a COVID-19 breakout in Malaysia, at the production plants for the world’s largest producer of gloves.
Early in the pandemic, some products, such as toilet paper and disinfecting sprays, were difficult to find. Have we learned anything from that?
Gupta: The toilet paper shortage arose due to unprecedented demand surges for a commonly used household product. The supply chains were a victim of their own efficiency, as any capacity that was seen as wasteful had been eliminated in order to reduce costs.
The supply chain for the COVID-19 vaccines is set up differently. It’s a short-term measure aimed to secure a sufficient supply of vaccines for the population. The manufacturers know how many doses they need to produce. The challenge, then, is how they produce those vaccines in record time, how they transport them securely and efficiently, and how they administer them, while minimizing any waste.
Robb Frederick
Director of Strategic Communications, Penn State Behrend